What is Sleep Apnea?
Obstructive sleep apnea (OSA) is the term for when the airway collapses, either partially or fully, while someone is asleep. This limits or blocks the ability for air to flow into the lungs. As the person continues to try and breathe, the airway constricts, no matter how hard they try to keep breathing. Once this happens, the person will change the position of their tongue and jaw so that the airway is now open. This usually is followed by the person gasping or snorting. Finally, the person affected will begin this process again, and again.
Nearly 80% of the people with sleep apnea have it and don’t realize it.
The effects of this are harmful. It not only makes it harder to breathe, which can be dangerous, but it also leads to less restful sleep. When the airways constrict, the brain “awakens” the person so that they are sleeping more lightly. Spurts of gasping and snorting can repeat hundreds of times throughout the night, disrupting sleep all around.
There are three main types of sleep apnea:
-
The most common form is OSA. With OSA, the muscles in the neck and airway relax, and the soft tissues narrow or close your airway. You can’t breathe, so you snore or snort and wake yourself from a sound sleep. You may not realize this, but it can happen over 30 times each hour. This type of sleep apnea is most commonly treated in our practice.
-
CSA occurs when the brain simply forgets to tell you to breathe. While it shares some causes with OSA, it may also relate to certain medications or having had a stroke.
-
Treatment-emergent sleep apnea is when you’ve been diagnosed with OSA, and during your treatment develop CSA. Some studies show that TECSA can occur at any CPAP setting although extremely high CPAP settings could increase the likelihood or persistent use of the CPAP can prolong risk OF TECSA.
Like many of life’s ailments, sleep apnea can be impacted by age, weight, family history, and your consumption of alcohol or medications. But it isn’t simply an old-age problem. You can develop sleep apnea at any age. While excess weight can exacerbate sleep apnea, it’s a contributing factor and not a determining one. And moderate consumption of alcohol and use of prescription medications may not lead to sleep apnea.
Simply being tired isn’t the only side effect of sleep apnea. It can cause headaches, shortness of breath, inability to focus during the day, and increase your risk of heart attack, stroke, and even Type 2 diabetes. Chronic facial pain such as, headaches, migraines, TMJ/TMD, are shown to often have a sleep disorder prior to the pain and treating the sleep disorder improves the pain.
Obstructive sleep apnea is treatable. The first step in the process is completing an evaluation which may include an easy at home sleep test. While there are complicated treatment options, like a CPAP machine or surgery, our experience and numerous studies have shown that the outpatient solutions that we offer can provide immediate relief.

Women from age 50 to 70 have a 3x greater risk of moderate to severe OSA than men.
Did you know that 25% of adults in the U.S. are estimated to suffer from sleep apnea. Sleep apnea is linked to obesity, diabetes, stroke, and heart failure.
For those who suffer from obstructive sleep apnea, it is nearly impossible to go through the full cycle of a restful sleep. There are four stages of sleep, and each one is necessary to achieve a full night’s rest.
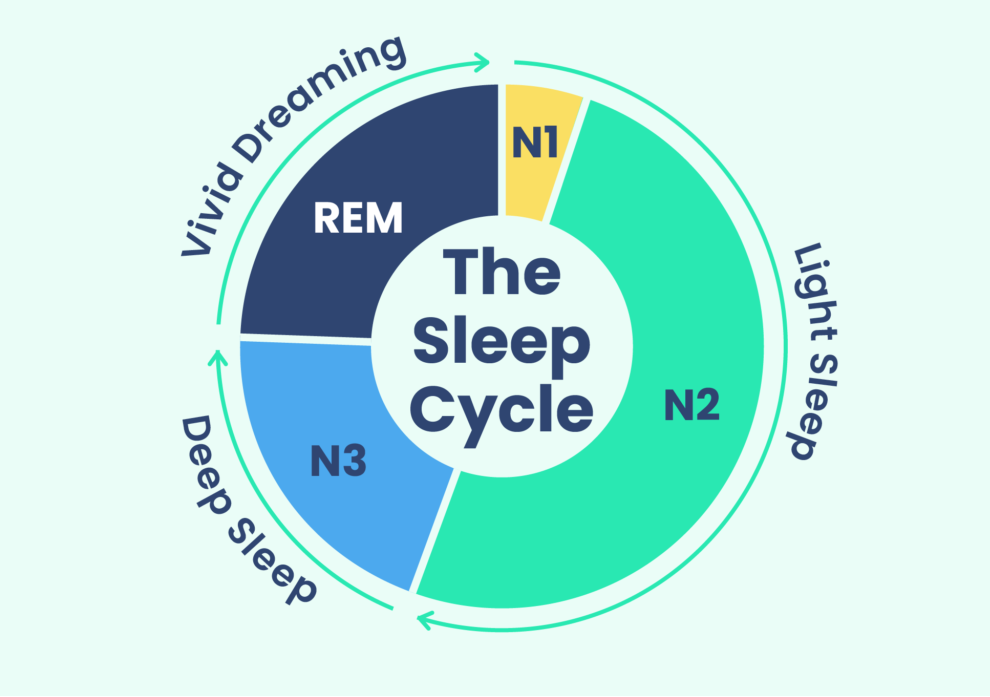
The four stages of the sleep cycle are:
Transition – about 5% of the total cycle.
Light – about 45% of the cycle.
Deep – about 25% of the cycle. This is when the body heals itself and many important reparative functions occur. People who don’t enter the deep cycle will be tired the next day.
REM – Rapid Eye Movement – about 25% of the cycle. This is when most memorable dreams occur. People who don’t complete a full REM cycle tend to complain that they are tired and find it difficult to concentrate.
What are the symptoms of sleep apnea?
It can be challenging to distinguish between obstructive and central sleep apneas since their signs and symptoms sometimes coincide. Obstructive and central sleep apnea's most typical warning signs and symptoms are as follows:
• A loud snore
• Episodes where you stop breathing while sleeping, which someone else might notice
• Breathing heavily when sleeping
• Dry mouth upon awakening
• Daytime headache
• Having trouble remaining asleep (insomnia)
• Excessive slumber during the day (hypersomnia)
• Inability to concentrate while awake
• Irritability
PAP Machine Therapy
Positive Airway Pressure (PAP) is the most common treatment for obstructive sleep apnea. Patients who receive PAP therapy cover their mouth and/or nose with a mask. . Air is gently blown via the mouth and/or nose using an air blower. The air pressure is set to exactly the right amount to keep the tissues in the upper airways from collapsing while you sleep.
The most popular PAP device is CPAP (Continuous Positive Airway Pressure). The machine has only one pressure setting.
Bi-Level PAP employs one pressure when you breathe in and a lower pressure when you exhale (breathing out). Before health insurance will pay for the bi-level, a requirement must be satisfied. This typically implies that before insurance will pay for a bi-level, the CPAP machine must be tried out first and proven to be ineffective, with the results being documented.Despite its widespread use, many people are CPAP intolerant and are unable to wear the mask at night due to how invasive and uncomfortable it can be.
Oral Appliance Therapy
A mandibular advancement device is one such oral appliance used in the treatment of sleep apnea. They are worn in the mouth overnight and look like sports mouth guards. Their purpose is to ease the lower jaw forwards with the use of metal or elastic hinges to make breathing easier.
Another is a tongue retaining device, which acts as a kind of splint to keep the tongue in place and open the airways.
Surgery
If needed, nasal surgery may help a patient’s ability to use a CPAP. Depending on the nature of obstruction, bimaxillary advancement and tracheostomy ( when a surgeon makes an opening in the front of the neck and inserts a tube into the windpipe to help patients breathe).